Surgical Treatment for Otitis Media
WHAT IS THE SURGICAL PROCEDURE FOR TREATING MIDDLE EAR INFECTIONS?
When middle ear fluid and infection fail to respond to medication, surgical therapy may be necessary. The most common surgery for middle ear disease involves the creation of a small incision in the eardrum called a myringotomy. Through this incision, the fluid within the middle ear space may be removed and any remaining fluid may be allowed to drain spontaneously. Of most importance, air from the ear canal may freely enter the middle ear space. This free entry of air effectively prevents vacuum formation as long as the myringotomy incision remains open.
In order to maintain an air passage through the eardrum long enough for the middle ear disease to resolve, an artificial device must be inserted in the eardrum to hold the incision open. The most popular device is the tube. It is given a variety of names such as the tympanostomy tube, the ventilation tube, and the pressure equalizing or PE tube.
After creation of the myringotomy incision, the tube is carefully inserted into the incision to hold it open using stereomicroscopic visualization. After the tube has been inserted, antibiotic drops or other medications are placed in the ear canal to prevent tube blockage or middle ear infection following the procedure.
The tubes themselves are small, about the size and shape of a capital letter "O" on this page. There is a large variety of commercially-made tubes available for use. Tubes vary in size, shape, and material. Each tube has been designed for particular clinical situations. All tubes are constructed of materials well-tolerated by the body.

T-Grommet tube
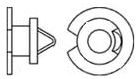
Paparella tube
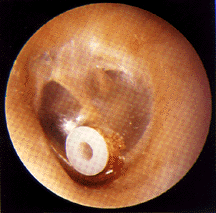
Tubes, when properly positioned, will not protrude from the ear canal nor will they fall through the incision into the middle ear. They normally will not be visible except with a special examining instrument, the otoscope. How long the tube remains in your child's eardrum depends upon many factors, including the thickness of the eardrum, the position of the tube placement, and the amount of eardrum growth during the time that the tube is in place. Tubes usually remain in place in the eardrum for an average of eight to eleven months. However, the tubes may fall out immediately after insertion or remain in place for over two years.
The tube seems to be pulled out of the eardrum by the slow growth of the eardrum skin. Eardrum skin tends to grow and seemingly move slowly from a point in the central portion of the eardrum out into the ear canal. The skin tends to carry the tube along as it moves. The tubes may plug with wax or crusts, particularly those which may form if an ear infection occurs while the tube is in place. When plugging occurs, the eardrum may stretch inward and close behind the plugged tympanostomy tube, forcing it out of the eardrum. Because the force of the eardrum tends to pull the tube outward, it neutralizes any tendency for the tube to fall into the middle ear.
Once the tube leaves the eardrum, the myringotomy incision usually closes within several days to weeks, depending upon how long the tube was in place. The tube itself may remain within the ear canal for months. Tubes often fall out of the ear canal by themselves or may be removed from the canal as part of an accumulation of ear wax. Tubes are usually painless while in the eardrum or after they have fallen out into the ear canal. The only way you know that the tube is in place is that your child will hear better and will probably have fewer ear infections. In some circumstances where the tube has been in the eardrum or within the ear canal for a prolonged period of time, it may induce a localized infection with pain, drainage, and sometimes bleeding.
WHAT ARE THE COMPLICATIONS OF TUBES?
A number of undesirable results may occur during or following a myringotomy with tube insertion. Complications may be associated with the general anesthesia administered to your child during the tube insertion. Anesthetic complications vary from region to region and may also vary with the general health of your child. Although published studies predict that anesthetic complications could occur in one of every thousand cases, I have not seen a life-threatening complication occur in any of my patients undergoing this type of surgery. I have, fortunately, never had to admit a child to the hospital for treatment of a complication related to insertion of tympanostomy tubes.
Bleeding or acute middle ear infections may immediately follow tube insertions. These problems may be controlled using ear drops, ear packing, and antibiotics taken by mouth or administered in ear drops. Late complications which have been "associated" with indwelling tubes include: infection with drainage through the tube, crusting and bleeding around the tube, persistent eardrum perforations, eardrum scarring, and eardrum retraction pocket or cholesteatoma formation. It must be stressed that these complications are "associated" with tube insertion and not necessarily caused by the operation or the indwelling tubes themselves. Many of the same complications are commonly seen in ears with recurrent or persistent middle ear infections or fluid and seem to be related to the severity and chronicity of disease rather than its treatment. In contrast, children who have had repeated and timely tube insertions quite often have normal appearing eardrums, even after having the insertion of many sets of tubes.
Tubes should not remain in the eardrums for more than two years to two and one-half years, since the risk of a permanent perforation increases after this period of time. Should a perforation occur and persist, it may be patched with a relatively straightforward surgical procedure.
In rare instances, particularly in ears which have sustained much eardrum damage, a tube may fall into the middle ear space rather than extrude out into the ear canal. In such cases, a tube remaining behind the eardrum has very little effect on middle ear structures or their function since the prosthesis is constructed of materials well-tolerated by the body. The tube is easily removed through an incision made in the eardrum.
WHY MUST TUBES BE INSERTED REPEATEDLY?
The insertion of a tube allows air to enter into the middle ear space permitting the middle ear linings to return to a normal state. This may help correct some eustachian tube functional problems relating to blockage at the “ear-end” of the eustachian tube. Problems occurring at the “nasal-end” of the eustachian tube, including muscle malfunctions which impede opening and closing of the tube and swelling or infection at the nasal end of the tube, will probably not be helped by the tube insertion. Unless problems at both ends of the eustachian tube resolve during that period while the tubes remain in place, middle ear disease will recur after the tubes extrude.
If middle ear disease does recur in such an instance, I may suggest more intense medical, surgical, or combination therapy for treatment of the recurrent disease. Recurrent disease in a child who has previously had tympanostomy tubes inserted will usually require reinsertion of the tubes. Of course, the time of year and the individual circumstances of the case will ultimately determine the timing and the choice of therapy.
ABOUT THE OPERATIVE PROCEDURE TO INSERT TUBES
The operative procedure is usually carried out in an ambulatory surgery suite. You and your child should arrive ONE TO ONE and ONE-HALF HOURS prior to the time the operation is scheduled to begin in order to allow sufficient time for necessary pre-operative discussions and examinations.
Prior to the surgery, you and your child will meet the anesthetist who will administer the anesthesia. We usually induce anesthesia in the operating room by having a child breathe “laughing gas,” nitrous oxide through a mask. The effect is prolonged and deepened using the safest anesthetic medications in use today, again administered through the same mask. A breathing tube and an intravenous are usually unnecessary due to the short duration of the anesthetic. Particularly anxious young children may be given a sedative for relaxation prior to entering the operating room. If your child is over the age of 12 months, one parent or designated family member will be permitted to accompany her or him into the operating room. You will be accompanied by a professional escort, a regular member of the operating room staff.
Once your child is asleep, the operation is performed using an operating microscope which magnifies the eardrum and other vital structures within the ear canal. The eardrum is incised with a microscalpel, and any middle ear fluid is suctioned out. The tube is inserted with microforceps by slowly rotating it into the incision. Ear drops are placed in the ear canal and allowed to enter the middle ear through the tube. In some children, certain specialized tubes may be used or oxygen inserted under pressure to return the eardrum to its normal position.
Following completion of the surgery, your child is awakened from deep anesthesia and returned to the recovery room. I will come to speak with you in the waiting area about the procedure. Once your child is settled in the recovery room, you will be asked to come in to be with your child during this awakening process. Be aware that most small children are very agitated when they awaken, chiefly due to disorientation from the anesthesia, but also due to the sudden appearance of loud sounds and some pain in the ears. This will improve as they awaken more completely, but their agitation will often continue until they leave the hospital, return home, and have a good, long nap. You will be given a recommendation for an enhanced dose of Tylenol to be used for control of pain. Do not use medications such as Advil™, Motrin™, or aspirin as they may cause bleeding.

WHY ARE ADENOIDS AND TONSILS SOMETIMES ALSO REMOVED
AS PART OF TREATMENT FOR MIDDLE EAR DISEASE?
Adenoid and tonsillar excision may help eliminate middle ear disease if there is evidence that these structures are contributing to spread of infection up through the eustachian tube. Recent controlled studies indicate that the routine inclusion of tonsillectomy along with tube insertion will not guarantee faster or more permanent resolution of middle ear problems. Adenoidectomy seems to have some utility in preventing the need for repeated reinsertion of tubes. For more information, click to my page "Role of Adenoidectomy in Treating Otitis Media."
ADENOIDECTOMY.
Adenoidectomy, when advisable, is performed on an ambulatory basis along with the tube insertions. The adenoids are a collection of white cells which migrate to the top of the throat behind the nose due to repeated nasal or throat infections or due to other stimuli such as allergies. They are removed from the upper throat or nasopharynx to improve the function of the eustachian tube and to eliminate a source of infection which may spread up into the middle ear spaces.
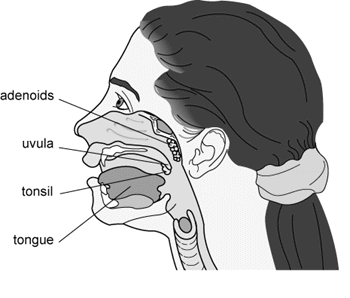
General anesthesia for an adenoidectomy requires the insertion of a breathing or endotracheal tube into the upper windpipe to allow safe and painless surgery with the child's mouth open. In contrast, the brief anesthesia for a tube insertion requires only a face mask since it is possible to cover the mouth and nose during this type of brief ear surgery. The passage of the endotracheal tube is a routine part of most general anesthetics, and it requires the insertion of an intravenous to allow for the administration of medications during a longer anesthetic.
Surgery is carried out through the mouth without the need for any external incisions. The mouth is held open by a surgical gag, and the tongue is depressed. Before the surgery commences, the soft palate is assessed for length, position, and muscular integrity. If I feel that the palate is currently using some of the adenoidal tissue to help it perform its “valve” function in the throat, I may elect to only remove a portion of the adenoidal tissues to prevent loss of effective closure of the upper throat during speaking and swallowing. Adenoidal tissue is removed using specially designed instruments which are able to reach up and back into the upper recesses of the throat.
WHAT ARE THE POTENTIAL COMPLICATIONS FROM ADENOIDECTOMY?
The major complication associated with adenoidectomy is bleeding from the operative site. This occurs most frequently either during the first two days or at six to ten days following the operation. Bleeding occurs when a small fragment of the scab or healing tissue dislodges and exposes a blood vessel beneath. Although most persistent bleeding is self-limited, we consider it to be a major complication requiring a doctor's examination and, in some cases, a return to the operating room.
Another potential complication is post-operative infection. This is usually manifest by significant, continuous headache, pain referring to the ears, or neck stiffness. If these symptoms occur, you should contact me at once. If an infection should occur, it may be necessary to change the antibiotic or increase the dose of the drug that your child is currently taking.
Removal of large adenoids may produce a temporary or, rarely, a permanent change in your child's voice or a tendency for fluids to leak into the nose when swallowing. This may occur because the enlarged adenoidal tissue may be aiding the soft palate in closing off the entry of air from the throat into the nasal cavity while speaking or swallowing. Prior to removal of the adenoids, I check the palate very carefully for evidence of insufficient length or position problems which might predispose to creation of this type of problem. If these exist, I will only remove the nonessential portions of the adenoidal tissues. Despite such precautions, difficulties may arise. If these problems do occur, they usually resolve spontaneously in several months. If they do not, an operation may be necessary to partially close the entrance into the back of the nose.
It is not unusual for adenoidal tissues to regrow, particularly in very young patients or in those patients who have allergies to inhaled materials. Should the adenoidal tissues regrow, they may be removed again. Usually, regrown adenoidal tissue is less abundant than the original adenoidal mass.
Scarring of the raw surfaces in the back of the nose occurs rarely after adenoidectomy. If it should, the scar could seal the entry way into the back of the nose. An operation would be required to reopen the nose.
Despite precautions, the instrumentation used in the performance of the operation may produce complications. The gag used to hold the mouth open must place some pressure on the tongue, lips and teeth. Occasionally, these tissue are unusually sensitive to this pressure. The tongue or lips may swell and become uncomfortable. Teeth, particularly first teeth, may loosen. It is common for the lips and tongue t0 feel uncomfortable over the first day or two following the surgery.
Blood vessels at the operative site may require sealing with an electrocautery device. Should the device malfunction, a spark may jump to tissues within other parts of the throat, mouth, or face and create a burn which could cause pain and scarring.
It is normal for there to be snoring an heavy breathing for the first week to 10 days following surgery. This will disappear once the palate swelling due to the surgery resolves.
PRE-OPERATIVE INSTRUCTIONS:
1. General anesthesia must be administered on an empty stomach. IT IS IMPORTANT THAT YOUR CHILD HAVE NOTHING TO EAT OR DRINK FOR FOUR TO EIGHT HOURS BEFORE THE SURGERY DEPENDING UPON THE AGE OF YOUR CHILD. If your child has anything to eat or drink, even water, too close to the surgery, the procedure will have to be cancelled for your child's safety. You will receive instructions the day before the surgery from the nurses at the hospital. Follow these instructions carefully.
2. A parent or guardian must accompany the child to the hospital. This person should be prepared to remain at the hospital during the procedure and for approximately one hour thereafter while the child awakens from anesthesia. If your child is also having an adenoidectomy, plan to remain at least two hours after.
3. Many parents find it convenient to bring along favorite coloring books and other play toys to keep their child occupied during the waiting period before the operation. Be aware, though, that the surgical suite has toys and video games which are designed to keep children of all ages engaged and entertained.
4. General anesthesia cannot be given if your child has a fever or symptoms of an upper respiratory tract infection, a “cold.” To do so would increase the risk of a post-operative pneumonia. If you must postpone your child's operation for this or any other reason, please call my office at least twenty-four hours in advance, if possible.
5. Aspirin, aspirin-containing products, and most NSAIDs including ibuprofen (Advil® or Motrin® ) interfere with the body's blood clotting mechanisms. Please do not administer any of these products to your child for two weeks prior to surgery. Use acetaminophen (Tylenol® or generic versions), for pain relief or fever control.
POST-OPERATIVE INSTRUCTIONS:
1. Water must not enter the ear canal as it will pick up bacteria from the canal and carry them through the tube into the middle ear space, possibly causing a middle ear infection. This may be accomplished by avoiding head submersion or by using molded ear plugs in conjunction with bathing caps or brightly colored sweat bands. You may arrange to have custom-molded ear plugs called “swim molds” made for your child. Our office has a list of facilities which fabricate these plugs. Until the plugs are available, a piece of soft cotton coated with Vaseline™ should be placed in the entrance to the ear canal to help repel water. Cotton with Vaseline™ will not maintain a watertight seal for swimming.
2. If water accidentally enters the ear canal because your child is accidentally splashed or the head is submerged and the swim mold falls out, use one dose of the prescribed ear drops, 4 drops, in the affected ear or ears.
3. Be prepared for some drainage of fluid from your child's ears for the first days after surgery. Ear drops have been placed in the child's ears at the time of surgery and these may continue to drain.
4. Occasionally there will be blood-tinged fluid draining from the ear. If this persists during the day of surgery or the blood-tinged fluid becomes more bloody, please notify me.
5. I will ask you to place eardrops in your child's ears for at least three days and often for up ten days following surgery. Usually 4 drops should be placed in each ear three times a day. Don't throw the bottle of drops away after this initial period of use. They may be used on a one-dose basis should water accidentally enter your child's ear. Most ear drops have a one year shelf life.
6. Your child should visit me two to three weeks after surgery to check tube function and to arrange a post-operative hearing test.
7. While your child has a tube in an eardrum, it is important to keep all follow-up appointments. Follow-up evaluation includes examination of the ear canals to ascertain the positions of the tubes and to be certain that the tube, a prosthetic device, is not creating a localized infection and damage to the eardrum. When the tubes fall out of the eardrums, it is necessary to be certain that the drum is healing normally. Even if you notice that the tubes have fallen out of your child's ears onto the pillow, water precautions should be maintained until your child has been checked to make certain that the eardrum hole no longer exists before resuming water-related activities unprotected.
8. Be on the lookout for drainage from your child's ears, particularly during "colds" or serious teething. If you notice drainage, begin the ear drops 4 drops 3 times a day and call me. I may wish prescribe an antibiotic by mouth and will arrange to see your child for followup following treatment.
9. Communications are important! If you have questions or concerns, I am available at all times to discuss these with you. Please call and leave a message at my office.

